Key Takeaways:
- HPV (human papillomavirus) is extremely common; there are specific types of high risk HPV that are associated with cervical cancer.
- HPV often has no symptoms, so it’s important to make sure you’re getting screened regularly.
- There are two effective ways to prevent HPV: the HPV vaccine and taking precautions in sexual situations (e.g. using condoms and getting screened for STIs regularly)
HPV infections are very common; in fact, most people will get HPV at some point in their lives. In many cases, it clears up on its own, but if you have a high-risk HPV infection, it needs to be followed up on and monitored, as a persistent HPV infection is the single most important risk factor in developing cervical cancer.
What is HPV?
HPV (human papillomavirus) is a virus that can increase the risk of cervical cancer. This is a group of 200+ related viruses, some of which are spread through vaginal, anal, oral, or skin-to-skin contact during sexual activity. HPV is very common – according to the Centers for Disease Control, nearly all sexually active adults will get HPV at some point in their lives. Some HPV types cause warts (e.g., on your hands and feet), while others cause infection. HPV infections that persist for several years can lead to cancers of the cervix, vulva, vagina, penis, anus, mouth, and throat.

Sexually transmitted HPV falls into two groups: low-risk and high-risk HPV, and within these groups, there are different types of HPV. High-risk HPV is routinely tested for as part of your cervical cancer screening (and based on your age/guidelines).
Low-risk HPV
Most types of low-risk HPV do not cause cancer and tend to resolve on their own. A few types of low-risk HPV (i.e., Types 6 and 11) can cause genital warts. While genital warts may not be pleasant, they can be treated.
High-risk HPV
There are about 14 types of high-risk HPV that can cause cancer if they are left to persist over time. Types 16 and 18 are associated with most HPV-related cancers. The twelve other high-risk types less commonly cause cancer, but are still considered high-risk and require appropriate care.
What causes HPV?
HPV is most commonly transmitted from one person to another through vaginal, anal, oral, or skin-to-skin contact during sexual activity. It is often asymptomatic, making it very easy to pass it on to someone else without knowing.
HPV can also remain dormant in the body for many years and show up again after several years of ‘normal’ tests. Depending on how your immune system is doing, an HPV infection can be more or less detectable in your cervical cancer screening. Even if you had an HPV infection many years ago – and several ‘normal’ or HPV-negative tests since then – this HPV infection can still reappear, often at times when your immune system is compromised or stressed.
Here are the different ways HPV can show up in your body and on screening tests:
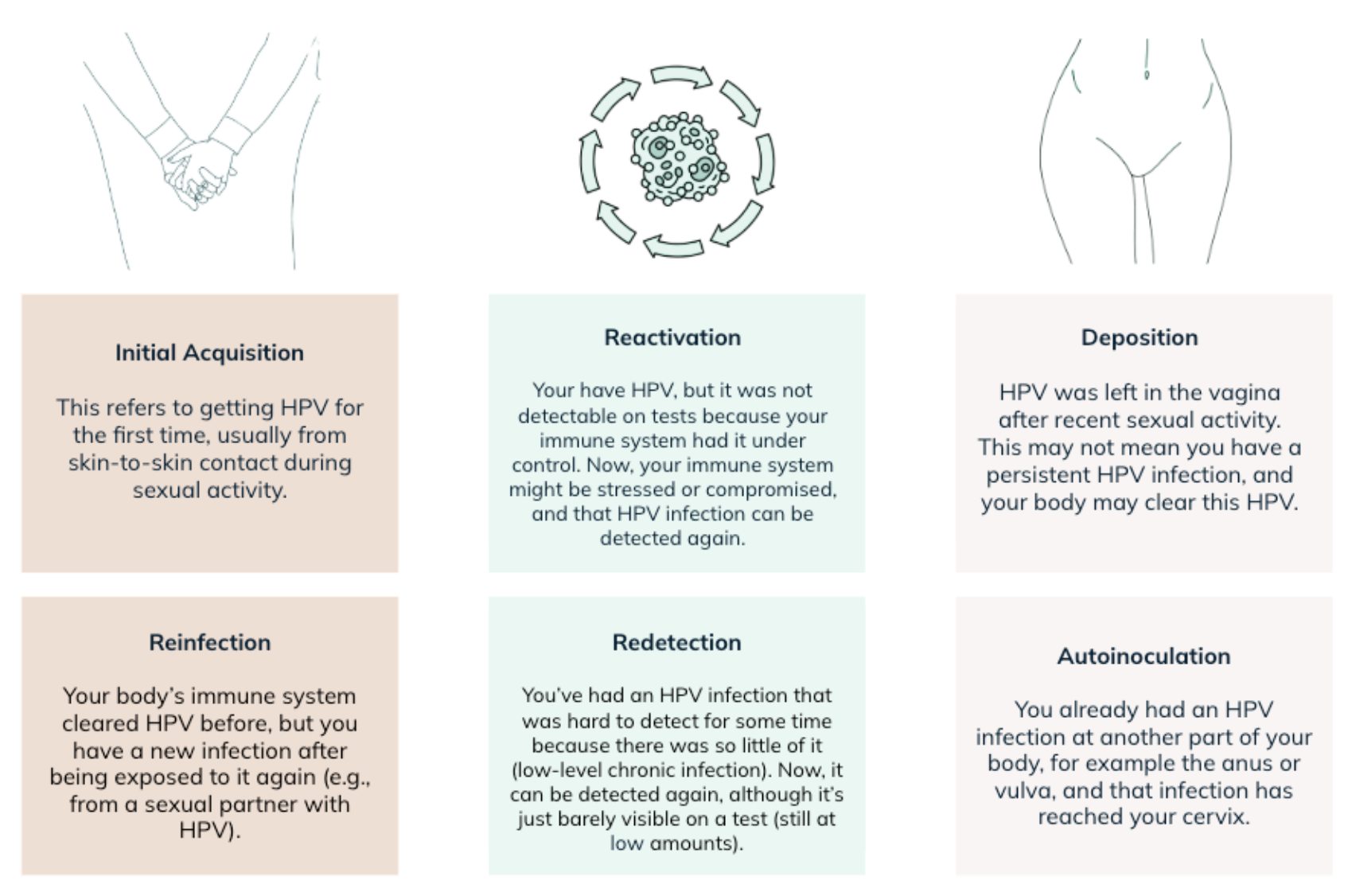
The changing nature of HPV is why it is so important to make sure you are getting screened when appropriate and medically recommended.
Does HPV always cause cervical cancer?
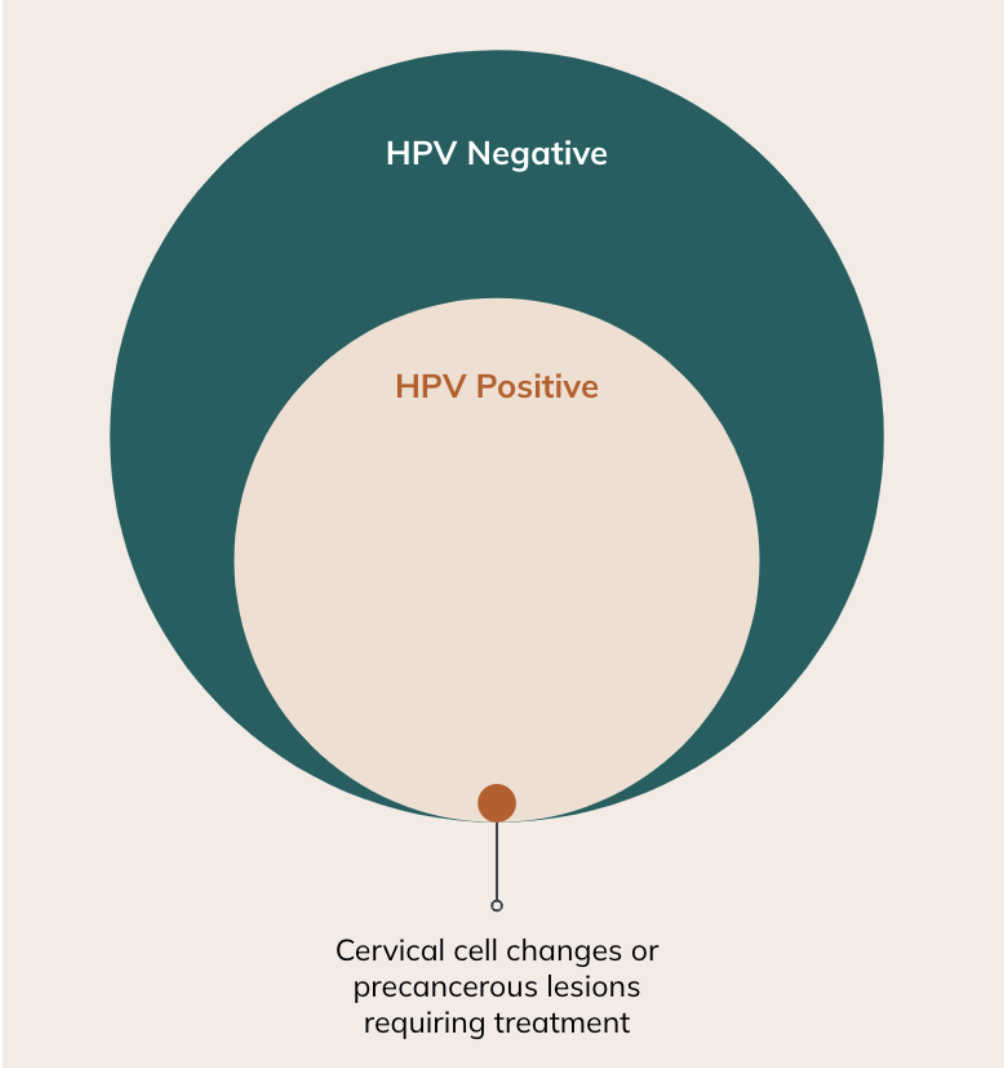
High-risk HPV types cause almost all cervical cancers; however, having an HPV infection does not mean you have cervical cancer. The infection must persist for several years before it causes cancer.
HPV is common, and typically, the immune system will clear the infection on its own within 2 years. This happens in most (around 90%) of cases. However, in those remaining 10% of cases, the HPV infection can persist. If an HPV infection goes without follow-up care for many years, it can cause abnormal cell changes that can lead to cervical cancer over time.
When HPV persists untreated, it takes about 5-10 years for HPV-infected cervical cells to develop into precancers, and around 10 years to develop from precancer into cervical cancer. However, abnormal cervical cell changes are easier to treat when they are identified early, and cervical cancer can be prevented entirely.
How can I protect myself against HPV?
Most sexually active adults in the US will be infected with HPV, so the best way to make sure an infection clears and does not lead to abnormal cell changes and cancer is to screen routinely based on recommended guidelines.
There is also a vaccine to help protect against HPV, however, this is most effective when administered before a person is exposed to HPV. The vaccine is routinely recommended for adolescents starting at ages 11-12 and can be given up until the age of 26. It is given as a 2- or 3-dose vaccination series depending on the starting age of vaccination. Some adults, ages 27 to 45, can also receive the vaccination, however, this may vary from person to person based on risk. To learn more, see our article on the HPV vaccine.
Practicing safe sex is important to reduce your risk of sexually transmitted infections (STIs), however, it doesn’t fully eliminate your risk of HPV because HPV can spread through sexual skin-to-skin contact as well. It is important to take precautions to reduce your risk of HPV by using condoms and getting regularly tested for STIs (and asking any sexual partners about their test results before having sex).
How is HPV treated?
Currently, there is no treatment for HPV, although in most cases, the body’s immune system will clear an HPV infection within a few years, without any treatment. In some cases, there may be treatments for the lesions (e.g., genital warts) that may arise from the HPV infection. Together with your provider, you can discuss a course of action that leaves you feeling more in control of your body and health.
The importance of cervical cancer screening
Screening for cervical cancer in women is the best way to prevent and diagnose high-risk HPV, which accounts for nearly all cervical cancers. When caught early, cervical cancer is curable 91% of the time.
When you screen with Teal Health using the Teal Wand, your sample is tested using an FDA-approved primary HPV test. The Teal Wand sample detects HPV-related cervical precancer 96% of the time, which is as accurate as samples collected by a clinician using a speculum and brush.
A primary HPV test is the most sensitive screening test for cervical cancer and is recommended by the American Cancer Society and the United States Preventive Services Task Force (USPSTF). The test looks for a current high-risk HPV infection, as sometimes these infections can be persistent, leading to precancerous cell changes and ultimately cancer.
Skip the stirrups
Get early access
Enter your email to get started.
$99 with insurance
$249 without insurance (reduced from $499)










